Survey of 730 clinicians shows factors other than compensation, such as autonomy, flexibility, and culture, are untapped competitive advantages employers should use to attract and retain talent
Conventional economics tells us that when demand outpaces supply, prices rise. That’s precisely what’s happening in the market for healthcare talent.
The prolonged shortage of healthcare talent is driving up the average provider compensation. While this affects every healthcare employer, it’s especially challenging for rural healthcare to address because they don’t have the volume of patients to make up the margin.
This means competing on compensation is a tough sell. Yet a new survey of 730 clinicians, including physicians and advanced practice providers (APP), suggests employers may not need to try.
The findings were detailed in a new report titled, Survey insights: What to know about the clinician workforce today. The report summarized the findings this way: “Meet the market on compensation. Outperform on schedule flexibility, work-life balance, and benefits.”
Provider job satisfaction does not help retention
The survey was conducted by the Advisory Board, a consultancy, and sponsored by LocumTenens, which specializes in placing temporary healthcare talent. The goal was “to learn about current job satisfaction, job preferences, compensation, and work environment.” The findings chart a path for employers to better compete for provider talent.
Overall, the providers who responded led researchers to three key findings:
- Compensation. Compensation is important, but other non-monetary factors play a significant role in attracting providers to an employer. This proved “true for clinicians at all stages in their careers” regardless of experience.
- Job satisfaction. Job satisfaction of providers is not a good indicator of employee loyalty. The report says, “Schedule flexibility and work-life balance can and do make up for lower pay.”
- No healthcare employer type has immunity. The type of employer had no impact on these findings. For example, while there are benefits and drawbacks to working for a corporate-owned hospital compared with an independent healthcare facility, the results were generally the same.
“Each type of employer has strengths and weaknesses that make them ‘the best’ for some clinicians, who have different priorities based on age, length of tenure, and other factors,” according to the report.
Effects on healthcare recruiting and retention
With all eyes on recruiting, healthcare employers also grapple with retention. This survey found 41% of responding providers intend to leave their current position within the next two years.
As with other aspects of the survey, this finding was persistent “across clinicians of all ages.” While about one in every two clinicians under the age of 40 expressed intent to change employers, the finding was also true for older providers. About one in three “clinicians in their 40s, 50s, and 60s were also considering leaving.”
Interestingly, job satisfaction was not correlated with job loyalty. For example, while more than three-fourths of providers (76%) said they were satisfied with their current position, of those, “28% are also considering looking for another position within the next two years.”
This is an important point because turnover adds cost for the employer. Institutional knowledge walks out the door, and it takes time, which in healthcare means lost revenue and additional capital to conduct a search for a replacement. Conservative estimates suggest a physician search costs $50,000 and takes several months to fill.
None of these points addresses the less quantifiable but just-as-important hidden costs of provider turnover. These include:
- institutional knowledge and experience walking out the door;
- onboarding and ramp-up time to get a new provider situated after an offer is accepted; and
- additional strain that is placed on the remaining providers to make up for the staffing shortfall.
These second-order effects add to provider burnout and put compounding pressure on recruiting and retention. It may sound folksy to say, but it’s true: If you want to refill a leaky bucket, the best place to start is by sealing the leak.
(Click to enlarge image)
What is it that healthcare providers want?
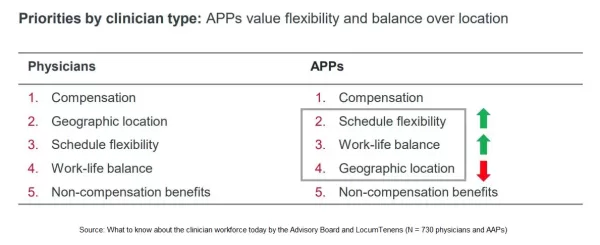
Broadly speaking, clinicians prioritized the same five factors in this survey when choosing an employer. While compensation is uniformly the top factor across all age groups, that’s just the stakes to get a seat at the recruiting table.
Differences emerge in several areas among the remaining four factors. These occur between physicians and APPs, generational cohorts, and among temporary staff, like 1099 providers fielded by LocumTenens.
For example, as the graphic nearby suggests, APPs, including physician assistants (PAs) and nurse practitioners (NPs), place more emphasis on flexible schedules and work-life balance. These are advantages where rural healthcare can outcompete urban facilities for talent.
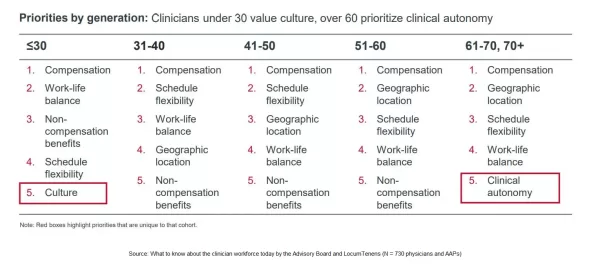
The report breaks out several other notable differences:
- Culture tops location for younger clinicians. The data shows that “for clinicians under 30, workplace culture replaced geographic location in their top five.”
- Location grows in importance with experience. “Location rises in importance with each subsequent age cohort — ranking second only to compensation for clinicians over the age of 51.”
- More experienced clinicians desire autonomy. Among clinicians ages 61 or older, “clinical autonomy replaced non-compensation benefits in their top five.”
- Contracted 1099 clinicians also value autonomy. The survey also found that providers working on a temporary, contract, or 1099 basis also put autonomy second on the list behind compensation.
The report sums up the findings with actionable advice: “While compensation consistently ranks first, organizations can outcompete on other factors.”
(Click to enlarge image)
Compensation alone is not enough to attract and retain talent
It’s clear from the data that compensation is “consistently prioritized compensation above all other factors.” The challenge here is that it will become “increasingly hard to out-pay competitors.”
To that end, the study also notes that competing on compensation alone is not enough to attract and retain talent. When the non-monetary factors are “taken together, schedule flexibility, work-life balance, and benefits outweigh compensation alone.” These are advantages that other healthcare industry surveys and observations suggest are organic to rural healthcare employment.
The report said this quite eloquently:
“Individually, these factors may not be enough to win talent, but delivering effectively against all three in combination can outweigh preferences for compensation — and outcompete organizations that rely on compensation alone to attract candidates.”
We’d hasten to add that the data suggests this is a healthy approach to also address the challenges of retaining healthcare providers.
* * *
See the software for yourself! Healthcare Workforce Management is designed with rural healthcare recruiting in mind because in our assessment, rural areas have the greatest need. Contact us for a no-obligation demo.
If you enjoyed this post, you might also like:
7 creative ways for rural healthcare employers to recruit providers
Image credit: Google Gemini